NEUPOGEN® is indicated for the mobilization of autologous hematopoietic progenitor cells into the peripheral blood for collection by leukapheresis.
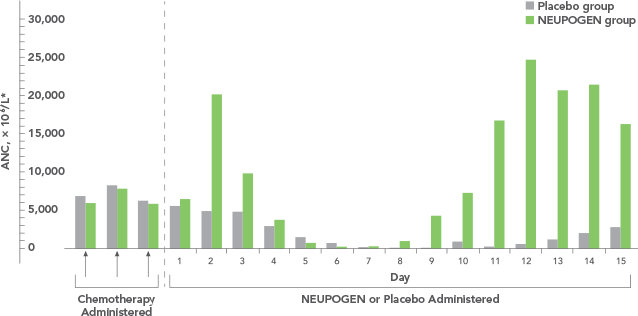
Daily NEUPOGEN, used to mobilize peripheral blood progenitor cell, reduced time to platelet and neutrophil recovery1,2
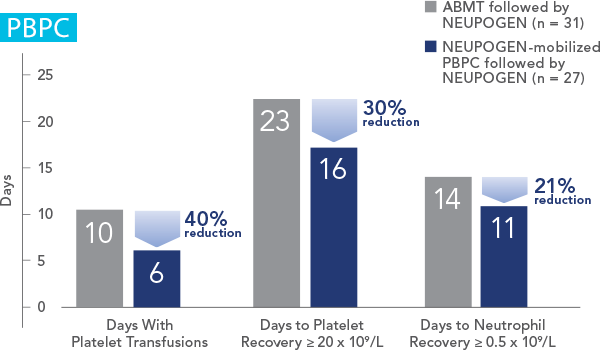
Median time to platelet and neutrophil recoveryMedian time to platelet and neutrophil recovery Expand Chart
Study design: A randomized, unblinded study of patients with HD or NHL undergoing myeloblative chemotherapy (Amgen study 3); 27 patients received NEUPOGEN-mobilized peripheral blood progenitor cell (PBCB) followed by NEUPOGEN, and 31 patients received autologous bone marrow transplant (ABMT) followed by NEUPOGEN. Primary endpoint was the number of days after PBPC transplantation or ABMT on which ≥ 1 platelet transfusion took place; secondary endpoints included time to achieve unsupported platelet count of ≥ 20 x 109/L and neutrophil count of ≥ 0.5 x 109/L.2
PBPC = peripheral blood progenitor cells;
ABMT = autologous bone marrow transplantation;
HD = Hodgkin's disease.
NEUPOGEN® (filgrastim) Prescribing Information, Amgen. Schmitz N, et al. Lancet. 1996;347:353-357.